To Health & Good Fortune in the New Year!
As you popped the Champagne and put oysters on ice to ring in the New Year, you may have wondered about your chances of shucking an oyster and finding a pearl inside. There are stories of this happening,1 but it’s incredibly rare. It’s thought that approximately one in 10,000 wild oysters yields a pearl;2 only a fraction of those, still, will be large and lustrous enough to make for a lucky find — your chances of this, it turns out, are about one in a million.3
Some pearls may develop in as little as six months.4 Yet, over time, as iridescent layers abound, they expand outward, growing in quality and value. As we reflect on the past year, one thing is clear: it has been a year of extraordinary growth and development for Pearl Health and value-based care. Below are some highlights from 2022 that leave us feeling like one in a million as we head into the new year. Cheers!
#1 Entering a New Era of Provider-Led Risk
The American healthcare system has always evolved along with shifts in social policy, market forces, and technological advances. Innovative value-based care programs, new risk-bearing entities entering healthcare, maturing capital markets, and increasing data interoperability are enabling a tectonic shift in healthcare spending and risk management.
This great risk shift from entities that traditionally bore healthcare costs (i.e. the government and insurers) to those who have traditionally been the providers and consumers of healthcare (i.e. doctors and patients) involves the transfer of risk related to $4 trillion (and more as time goes on) of healthcare expenditures.
Earlier this year, the Centers for Medicare and Medicaid Services (CMS) created the new ACO REACH model “to improve the quality of care for people with Medicare through better care coordination, reaching and connecting health care providers and beneficiaries, including those beneficiaries who are underserved….”
At Pearl Health, we believe value-based care models, like ACO REACH — along with supporting technology to enable effective risk management and care coordination across patient populations — have the potential to both increase the sustainability of our healthcare system and to align providers with their patients in a way that results in better care and more financial reward flowing to those who coordinate it.
We’re excited by the knowledge that is starting to come from the standardization of massive stores of previously non-interoperable healthcare data and the impact that increased data access and portability will have on our ability to generate insights that enable providers to deliver better care and succeed in this new era of provider-led risk management.
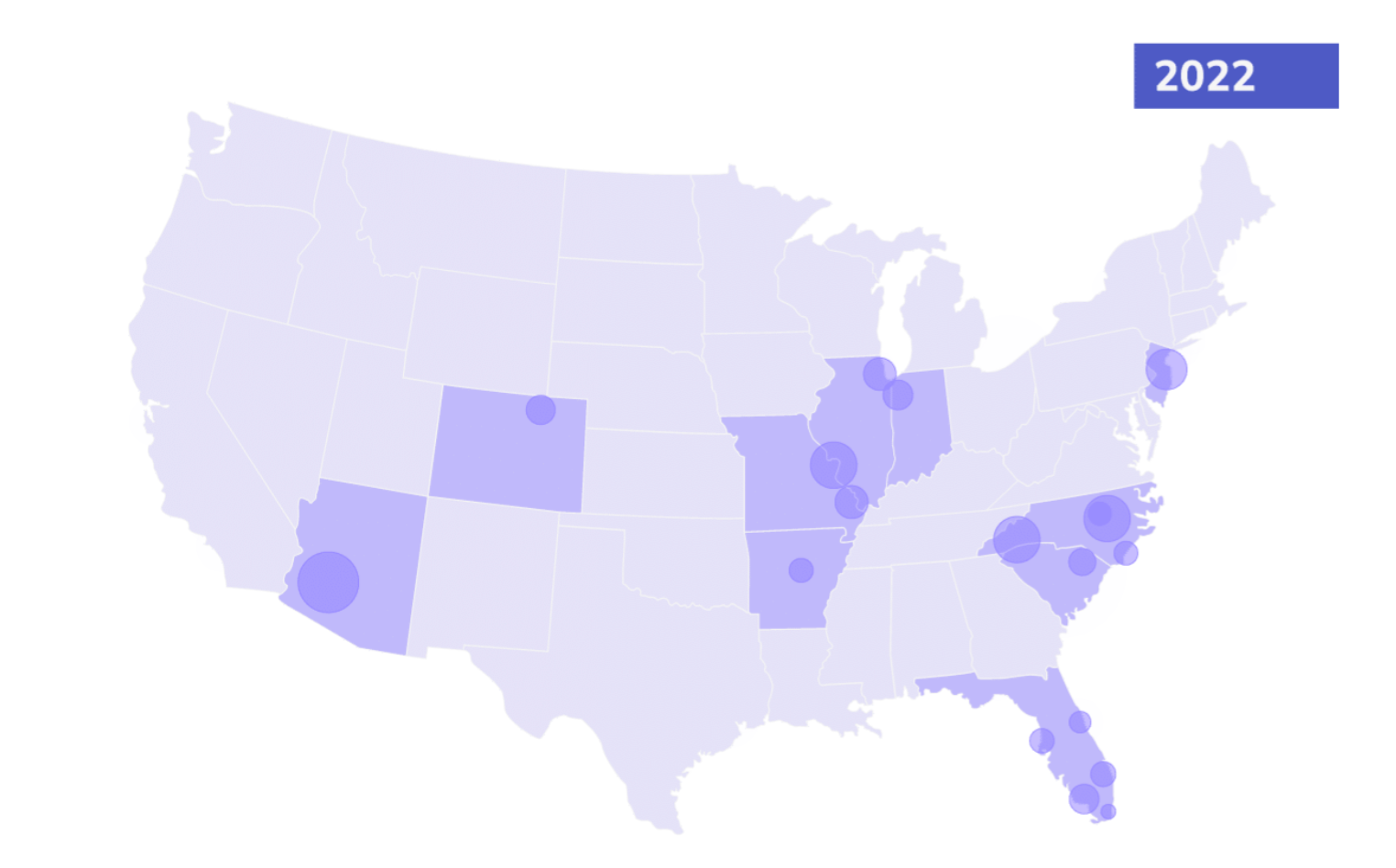
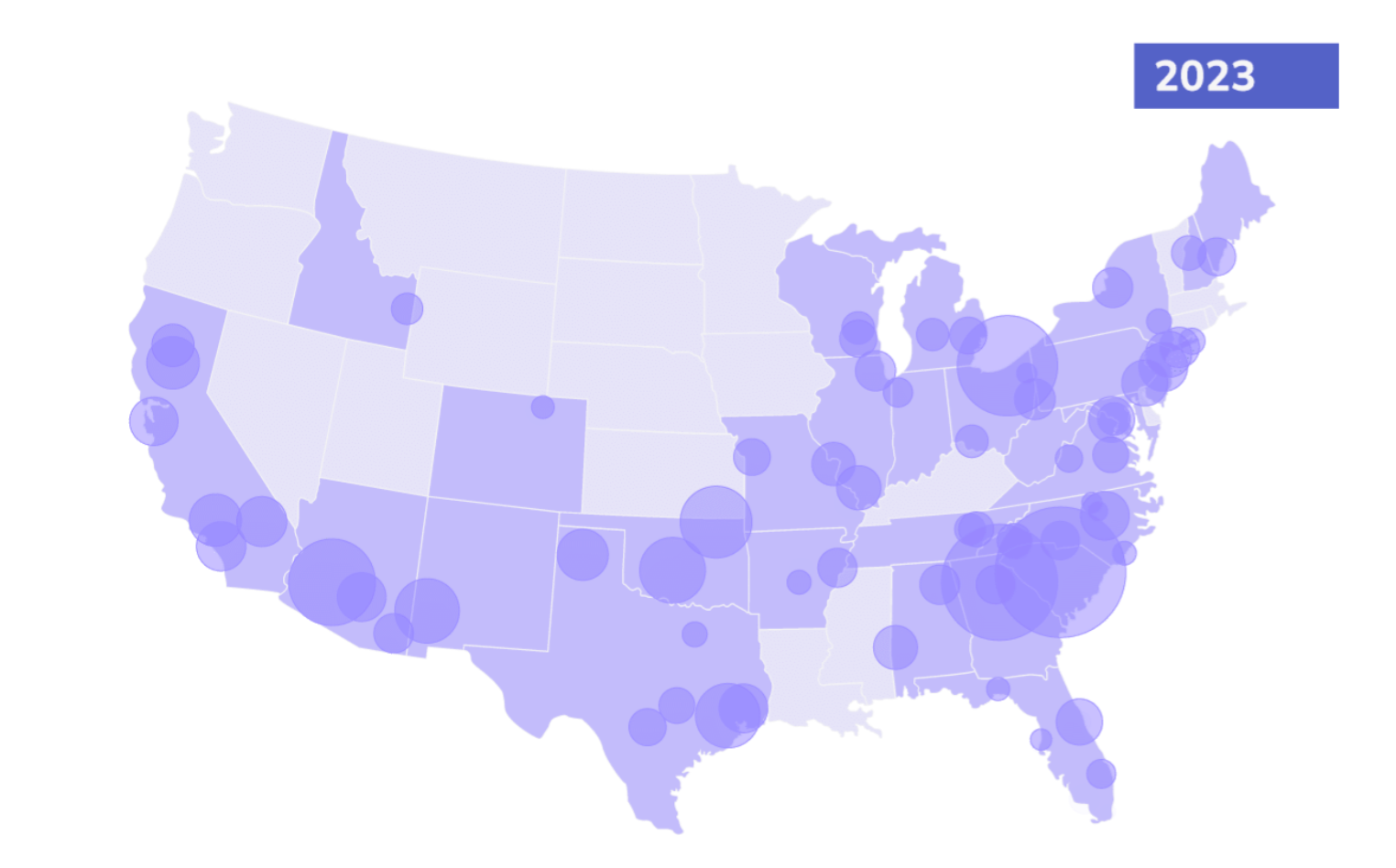
In 2022, more than 800 primary care providers from coast to coast partnered with Pearl Health, resulting in more than 10x year-over-year growth and expanding our network from 10 to 29 states.
From small independent PCPs to large groups, the rapid expansion of the Pearl Community reflects the growing appetite for participation in innovative value-based care programs. It also reflects Pearl’s deep commitment to enabling primary care organizations to transition from volume-based fee-for-service payments to value-based care with incentives aligned with keeping patients healthy.
We’re delighted to welcome these new partners to our Community and excited to help them develop care models that put patient- and provider-experience first and allow them to focus on delivering the highest quality of care.
#3 Improving Providers’ Prospects
At Pearl, we believe that innovative value-based care models, like ACO REACH, not only have the potential to improve patient experiences and outcomes: they also present opportunities for PCPs to increase and stabilize revenue and generate shared savings for their practices.
Yet, many primary care organizations lack the analytics capabilities and know-how to understand their options for participating in capitation payment programs, making potential risks and rewards opaque.
Earlier this year, we developed the self-serve Value-Based Care Advisor tool to provide transparency, help PCPs identify opportunities, and make it easy to understand the financial implications of participating in the model before diving in.
Early this year, we announced the launch of the Pearl Platform, technology purpose-built to enable PCPs and clinical staff with insights to proactively manage Medicare patient panels with less work, while surfacing org-level performance trends to deliver higher-quality care at a lower cost and drive continuous improvement.
In 2022, our team developed proprietary data science models that distill complex information across providers and facilities into what’s most important to enable proactive, whole patient care. We also developed several ways to visualize data to provide simple, actionable insights, including:
- A panel overview that gives providers and clinical staff a powerful heatmap to visualize risk, forecast patient needs, and identify the patients most likely to need attention;
- Detailed patient-level information with data across providers and facilities to provide holistic, longitudinal visibility;
- Alerts to enable timely clinical interventions, help manage transitions in care, and avoid readmissions;
- Turnkey reporting to provide strategic visibility into the most important determinants of success in Medicare’s REACH model.


As early adopters engaged with our product and took first actions across their patient panels, our team measured progress, took a principled approach to evolving the Pearl Platform, and prioritized building experiences that surface actionable information in low-friction, easily-consumable ways.
We’re proud to report that more than 3,000 actions were taken by the platform’s early adopters in 2022 and 60% of Medicare patients in the platform had actions logged by PCPs or clinical staff. As of December 2022, Pearl’s NPS score from early adopters is a staggering 94.4.
We’re extremely grateful to the providers and staff who partnered with us in 2022 to develop and refine the Pearl Platform and we’re excited to continue evolving with you to generate increasingly helpful patient and performance data in the year ahead.
#5 Growing a One-in-a-Million Team
As we have partnered with more and more primary care organizations across the country and invested in the scalability of our products and services, the Pearl team has been growing rapidly. In 2022, our team more than doubled, growing from 25 employees at the start of the year to more than 60 in January 2023.
In 2022, we’re delighted to have welcomed several senior leaders who have already made significant impacts in our ability to diversify our partnerships and offerings, accelerate product development and innovation, and create scalable systems that position us for rapid growth.
Pearl Leadership Hires in 2022

Pearl is led by provider-enablement, risk-bearing, and technology experts who are thoughtfully building a mission-driven team to democratize access to value in healthcare.
We’re still rapidly expanding across functions, including engineering, product, sales, marketing, customer success, and operations.
Interested in joining a one-in-a-million team in 2023? Check out opportunities on our Careers Page.