If you are reading this as a health system executive, you likely do not need another abstract case for value-based care. You are already living the reality behind the numbers.
Margins remain under sustained pressure. Labor costs continue to rise faster than reimbursement. Medicare and Medicaid now comprise the majority of revenue for many systems, steadily eroding the cross-subsidization model that underpinned hospital economics for decades. At the same time, expectations from patients, regulators, boards, and communities continue to escalate.
This article is informed by a recent conversation I had with Dr. Dennis Weaver, Chief Clinical Officer at Pearl Health, and Dr. Cameron Berg, EVP of Clinical Strategy at Pearl Health. Together, we explored why value-based care has proven so difficult for health systems to operationalize and why advances in artificial intelligence and other technologies may finally begin to change that equation.
What emerged was not a critique of health system leadership. It was a shared recognition that many of the decisions shaping today’s operating models were rational, even optimal, under a prior economic reality, and that those same decisions are now colliding with a fundamentally different one.
The Economic Reality Health Systems Are Navigating
For decades, health systems optimized for volume. Expanding access points, feeding high-acuity specialty care, and maximizing commercial reimbursement were sensible strategies. Commercial margins absorbed government losses, and modest surplus covered inefficiencies. As Dr. Weaver put it during our discussion, “Health systems were designed to maximize volume in their highest-margin, most clinically complex patients. That architecture made sense historically, but it’s now under real economic pressure.”
That pressure is measurable. According to the Medicare Payment Advisory Commission (MedPAC), hospital margins on fee-for-service Medicare have been consistently negative for more than 15 years, even during periods when overall all-payer margins appeared stable. In its most recent March Report to the Congress: Medicare Payment Policy, MedPAC estimates that aggregate Medicare hospital margins remain deeply underwater and are projected to stay negative absent meaningful structural change in care delivery and cost structure.1
Importantly, MedPAC’s analysis underscores that these negative margins are not driven by short-term volatility alone. Hospital input costs, particularly labor, pharmaceuticals, and supplies, have increased at rates that far outpace Medicare payment updates, which are tied to statutory formulas rather than underlying cost trends. MedPAC notes that while some hospitals temporarily benefited from pandemic-era relief and pricing adjustments, those effects have largely dissipated, leaving the core mismatch between reimbursement and cost unresolved.
At the same time, payer mix has shifted dramatically. As Medicare and Medicaid account for a growing share of total revenue, health systems have fewer opportunities to offset government losses with commercial margins. The historical cross-subsidization model that allowed systems to tolerate inefficiency and excess utilization has steadily eroded, exposing the underlying economics of care delivery in ways that are difficult to ignore.
Why Value-Based Care Stalls Inside Traditional Operating Models
A common executive concern is that value-based care introduces financial risk into already fragile organizations. That concern is valid.
The challenge, however, is that the underlying operating model was not designed for longitudinal, population-based care. Commercial populations are largely episodic, where improving value often means shifting site of service. Medicare populations are different. They are dominated by chronic disease, multimorbidity, and ongoing care needs.
Dr. Weaver framed it this way: “Value-based care works best where chronic disease dominates, which is why Medicare is the natural place for these models to succeed.”
Not all leaders agree. Many health system executives point out that Medicare Advantage penetration varies widely by geography, and that fee-for-service Medicare still underpins a significant share of hospital revenue. Others note that inpatient infrastructure cannot be unwound quickly without destabilizing access.
Those perspectives are reasonable. What is changing is the margin reality. As Dr. Berg noted, “When government payors dominate, success depends on preventing unnecessary care rather than optimizing around it.”
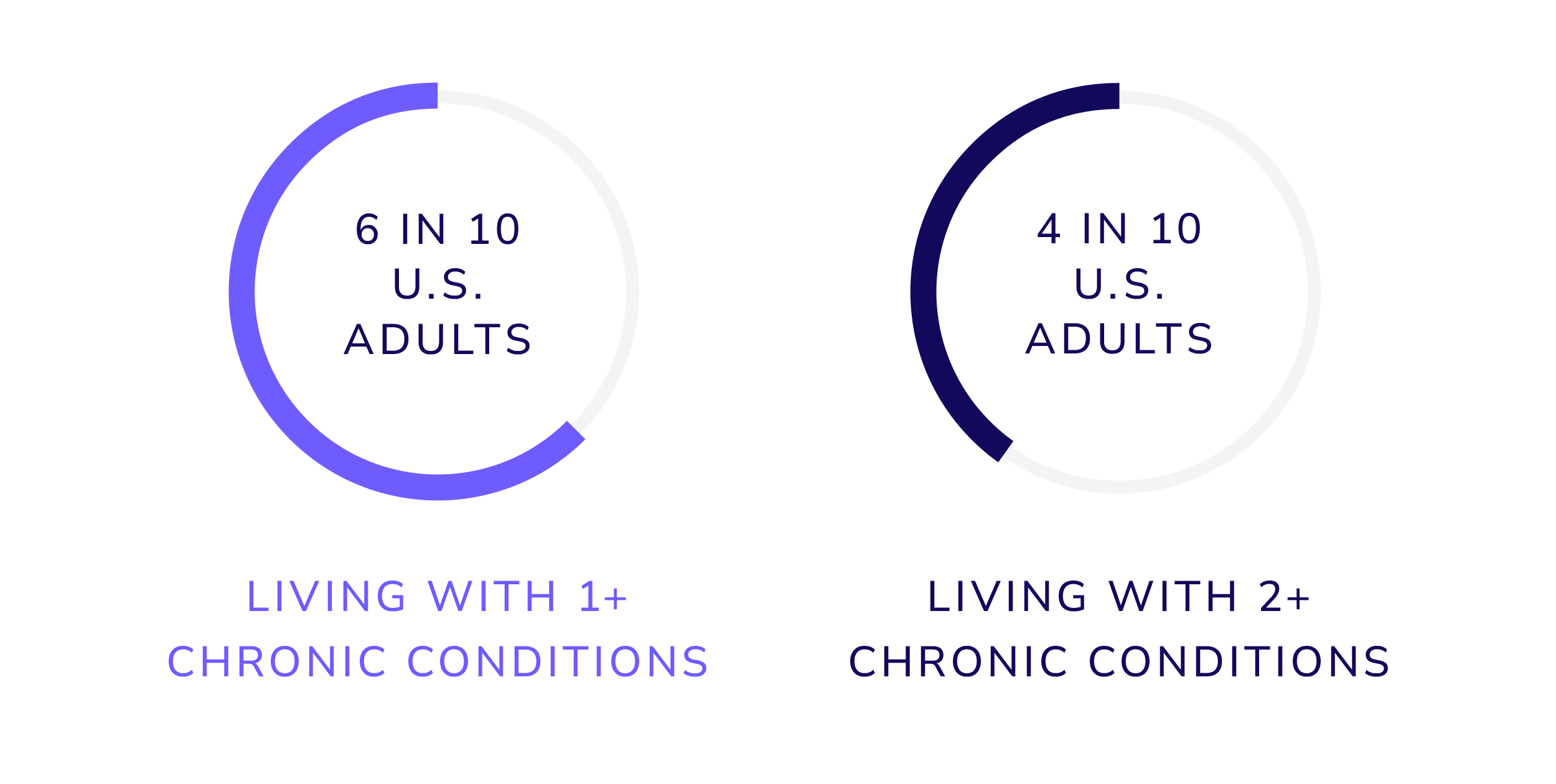
The CDC estimates that six in ten U.S. adults have at least one chronic condition, and four in ten have two or more2. Preventing avoidable exacerbations in these populations is no longer an abstract quality goal. It is increasingly a financial necessity.
Why AI Changes the Equation in Practice
AI is often framed as transformational or disruptive. In reality, its most powerful contribution is practical. As Dr. Berg shared, the shift is not just automation, but intelligence: “AI allows health systems to move beyond episode-based logic and toward person-level understanding of patient needs.”
This enables three critical capabilities.
- First, earlier and more precise identification of risk. McKinsey estimates that predictive analytics and AI-driven interventions could reduce U.S. healthcare spending by up to $450 billion annually, largely through earlier intervention and avoided acute episodes.3
- Second, better prioritization of action. Rather than static pathways, AI can help determine which patients need outreach now, which interventions matter most, and which can safely wait. The National Academy of Medicine has identified this as foundational to high-value care.4
- Third, expanded clinical capacity without expanding headcount. Labor remains the binding constraint for most systems. The American Hospital Association reports hospital labor expenses have increased more than 20 percent since 2019.5
Dr. Weaver summarized the operational implication clearly: “Traditional care management models don’t scale economically. Technology has to expand the reach of clinical teams without expanding headcount.”
For many health system leaders, this is both the promise and the tension of AI. The opportunity to extend clinical capacity is compelling, particularly in an environment where hiring additional staff is neither feasible nor sustainable. At the same time, executives are right to approach this shift with caution.
Concerns around algorithmic bias, clinical trust, data integrity, and regulatory scrutiny are legitimate. AI cannot function as a black box, nor can it sit outside established clinical governance. For these tools to deliver value, they must be transparent in how decisions are informed, accountable to clinical leadership, and designed to support, rather than supplant, clinician judgment.
Equally important, AI must be embedded directly into existing workflows. Layering new tools on top of already fragmented systems risks adding friction instead of reducing it. When thoughtfully integrated, AI can remove administrative burden, surface the right information at the right time, and enable care teams to operate more effectively at scale. When poorly integrated, it becomes yet another demand on limited manpower and capacity.
The distinction matters. Executed well, AI helps health systems optimize clinical capacity and improve consistency of care. Executed poorly, it reinforces skepticism and slows adoption. The path forward requires disciplined implementation, clinical partnership, and a clear focus on solving real operational problems rather than deploying technology for its own sake.
Patients Have Changed Too

Another assumption that deserves re-examination is patient digital readiness. Pew Research shows that more than 75 percent of adults aged 65–74 use smartphones today6. These patients are accustomed to on-demand information, digital self-service, and proactive communication in nearly every other aspect of their lives, and healthcare is no exception.
Dr. Weaver challenged the lingering misconception directly: “The assumption that Medicare patients aren’t digitally native is increasingly wrong. They expect answers when they need them, not the next business day.”
For health systems, this shift has real operational implications. Patient expectations are moving faster than traditional access models can accommodate. Call centers, care managers, and clinical inboxes were not designed to handle continuous, real-time engagement at scale, particularly as patient panels grow more complex and staffing remains constrained.
Meeting these expectations with human-only models is increasingly unrealistic. AI-enabled engagement offers a complementary layer that can triage questions, surface issues that require clinical escalation, and provide timely guidance outside of normal business hours. When thoughtfully implemented, these tools do not replace human relationships. They protect them by ensuring that clinical teams spend their time where it matters most, while patients receive responsive, consistent support.
In this context, digital engagement is no longer a “nice to have” or a generational experiment. It is becoming a foundational component of how modern care models maintain access, continuity, and trust at scale.
From Point Solutions to Operating Model Change
Health system leaders are rightly fatigued by disconnected point solutions. Over the last decade, many organizations have layered on tools to address specific problems, whether in care management, quality reporting, analytics, or patient engagement. Each solution often solved a narrow need, but collectively they added complexity, cost, and operational burden without fundamentally changing outcomes or economics.
What emerged clearly from our conversation is that sustainable success requires integrated change rather than incremental tooling. As Dr. Berg observed, “Health systems don’t need more point solutions. They need integrated approaches that improve outcomes while also improving margins.”
This is where perspectives sometimes diverge, and understandably so. For many executives, incremental optimization has historically been the safer path. Small improvements in throughput, length of stay, staffing ratios, or site-of-service mix could preserve margins without introducing significant operational risk. In relatively stable markets, that approach may still be viable.
However, in markets experiencing rapid payer mix shift, persistent workforce scarcity, and sustained margin compression, those levers are increasingly exhausted. Incremental gains can slow deterioration, but they rarely change the trajectory. Operating models designed for episodic, volume-driven, specialty focused care struggle to support longitudinal, prevention-oriented populations at scale.
The implication is not that health systems should abandon caution. Rather, it is that the nature of change required is evolving. Integrated models that align data, analytics, workflows, and clinical accountability around population-level outcomes offer a path to improve performance without layering additional complexity on already stretched organizations.

Where Pearl Fits and How We Engage
At Pearl, we work alongside health systems and physician organizations that are navigating this transition in real time. Our role is not to prescribe solutions from the outside or to advocate for technology in search of a problem. Instead, we partner closely with leadership teams to align data, clinical models, workflows, and AI-enabled execution in ways that reflect each organization’s strategic priorities, market dynamics, and operational constraints.
In practice, that means starting with the realities health systems face today. Fragmented data. Fixed-cost infrastructure. Workforce limitations. Regulatory complexity. Competing priorities across service lines. Any approach that ignores those constraints is unlikely to succeed, no matter how elegant it looks on paper.
We believe the organizations that succeed in value-based care will be those that can:
- Identify the right patients earlier, using longitudinal insights rather than retrospective reporting
- Intervene intelligently and efficiently, prioritizing actions that meaningfully change trajectories
- Reduce avoidable utilization without restricting access, preserving trust with patients and communities
- Improve margins while improving outcomes, aligning clinical and financial performance rather than trading one off against the other
Achieving this requires more than technology. It requires operating model change, clinical leadership, and a willingness to rethink long-standing assumptions about how care is delivered and supported. That work is difficult. It demands trust, iteration, and realism about what can change quickly and what cannot.
As Dr. Berg observed during our conversation, “Most health systems recognize the problem, but few have the internal technical capability to solve it alone.” That gap is not a failure of leadership. It is the natural result of organizations that were built to deliver care, not to design and maintain complex data and AI infrastructure.
Pearl’s role is to help close that gap in partnership with health system teams, bringing the tools, experience, and operating discipline required to turn value-based care from an aspiration into a durable capability.
If you are wrestling with how to make value-based care viable in today’s economic reality, we would welcome the conversation. Not as vendors, but as thought partners committed to designing what comes next together.
Connect with Steven Duque, Dr. Dennis Weaver, and Dr. Cameron Berg — and follow Pearl Health — on LinkedIn.
- Medicare Payment Advisory Commission (MedPAC). March 2025 Report to the Congress: Medicare Payment Policy. Washington, DC: MedPAC, March 2025. Available at: https://www.medpac.gov/document/march-2025-report-to-the-congress-medicare-payment-policy/
- Centers for Disease Control and Prevention (CDC), Chronic Diseases in America, indicating that approximately 6 in 10 U.S. adults have at least one chronic condition and 4 in 10 have two or more, available at https://stacks.cdc.gov/view/cdc/61396
- McKinsey & Company, The Big Data Revolution in Healthcare: Accelerating value and innovation (estimating that big data analytics/predictive insights could reduce U.S. healthcare spending by $300 – $450 billion), available at https://www.mckinsey.com/~/media/mckinsey/industries/healthcare%20systems%20and%20services/our%20insights/the%20big%20data%20revolution%20in%20us%20health%20care/the_big_data_revolution_in_healthcare.pdf
- National Academy of Medicine — Artificial Intelligence in Health Care: The Hope, the Hype, the Promise, the Peril 🔗 https://nam.edu/publications/artificial-intelligence-in-health-care-the-hope-the-hype-the-promise-the-peril/
- American Hospital Association (AHA). Fast Facts on U.S. Hospitals, 2026. Chicago, IL: American Hospital Association. Available at: https://www.aha.org/statistics/fast-facts-us-hospitals
- Pew Research Center, Mobile Technology and Home Broadband 2021 (showing that 71 % of U.S. adults aged 65–74 own a smartphone), available at https://www.pewresearch.org/internet/2021/06/03/mobile-technology-and-home-broadband-2021/





