Proving the "Pearl Effect"
To understand whether differences in outcomes reflect real performance variation or result from other factors, we evaluated two cohorts: a 2023 cohort over two performance years and a 2024 cohort observed over one. Each was compared against national trends from a large, randomized population of traditional Medicare beneficiaries. We focused on these timeframes because they represent the longest complete claims windows for which Pearl has data available at the time of analysis.
We then applied standard statistical controls, including a Difference-in-Differences (DiD) framework and Hierarchical Condition Category (HCC) risk adjustment to isolate performance shifts from external factors. The intent was straightforward: to ensure that observed improvements reflect changes in care delivery rather than differences in patient mix or broader market dynamics.
Rising Above the National Trend
Across four critical metrics, Medicare Beneficiaries aligned to providers on Pearl’s platform showed the same emerging pattern: early improvement, followed by a widening breakaway from the national average.
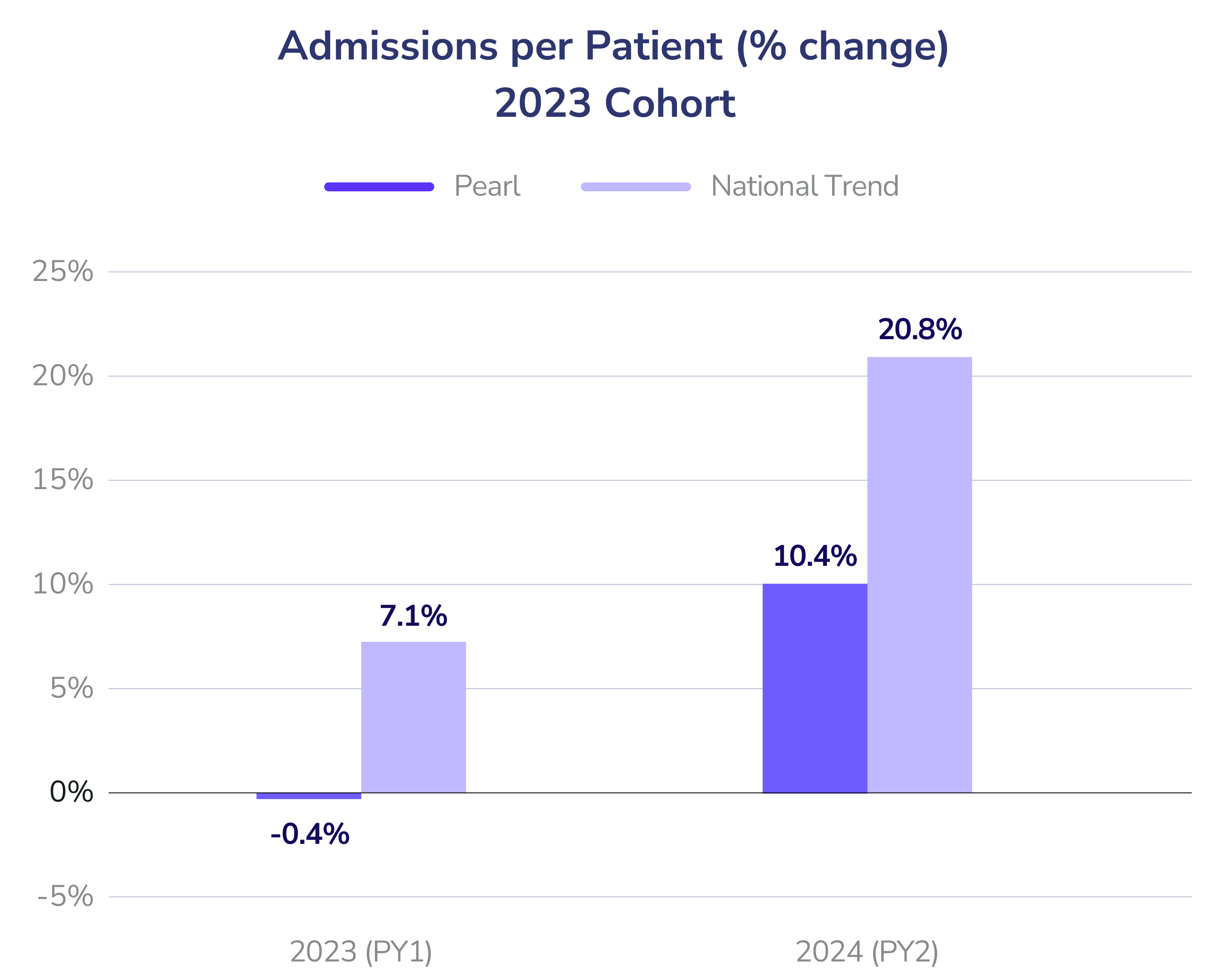
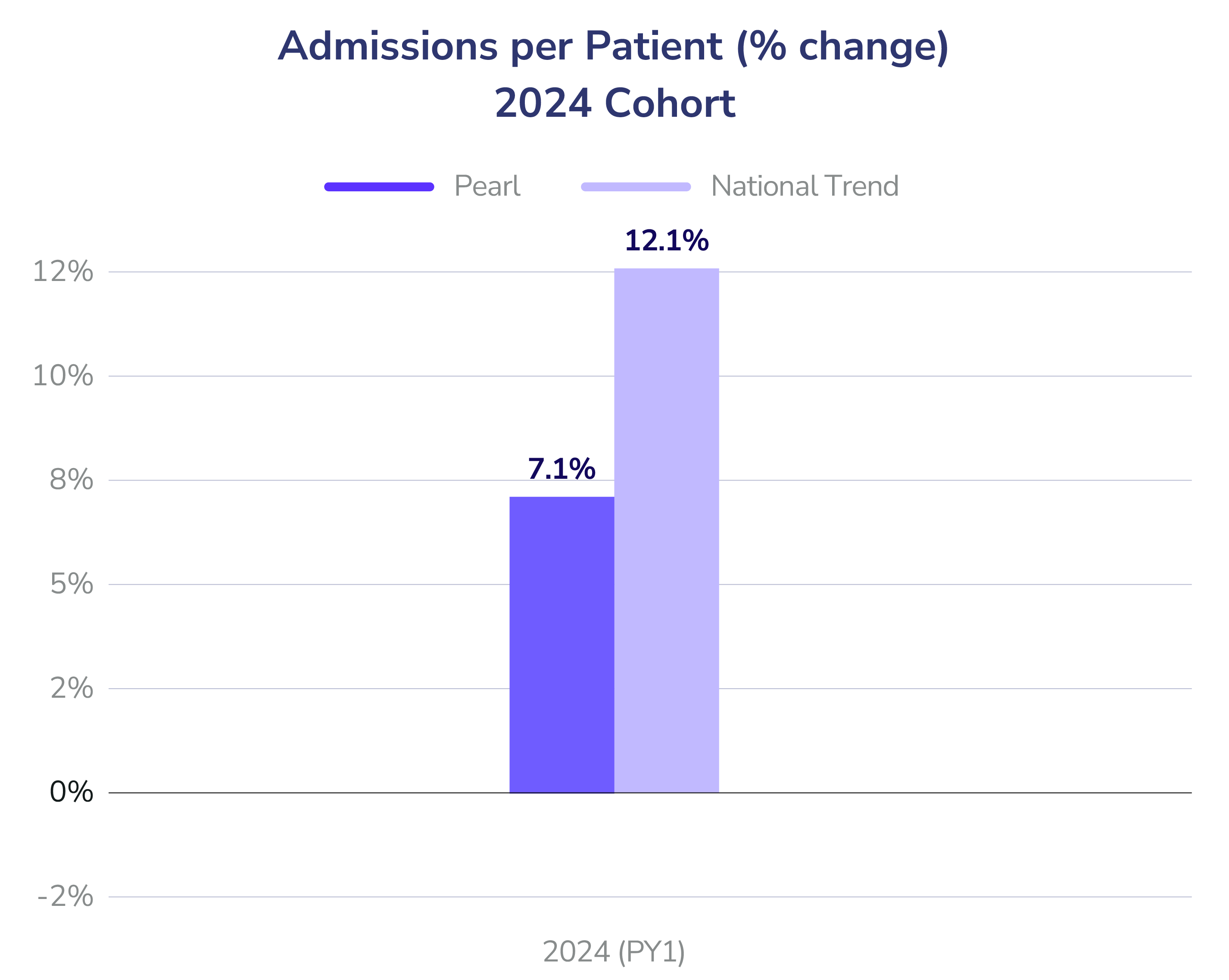
- Hospital Admissions per Patient: In Year 1, Pearl reduced admissions by 8% (2023 cohort) and 5% (2024 cohort) relative to national trends. By Year 2, our 2023 cohort accelerated those gains, reducing admissions by 10%.
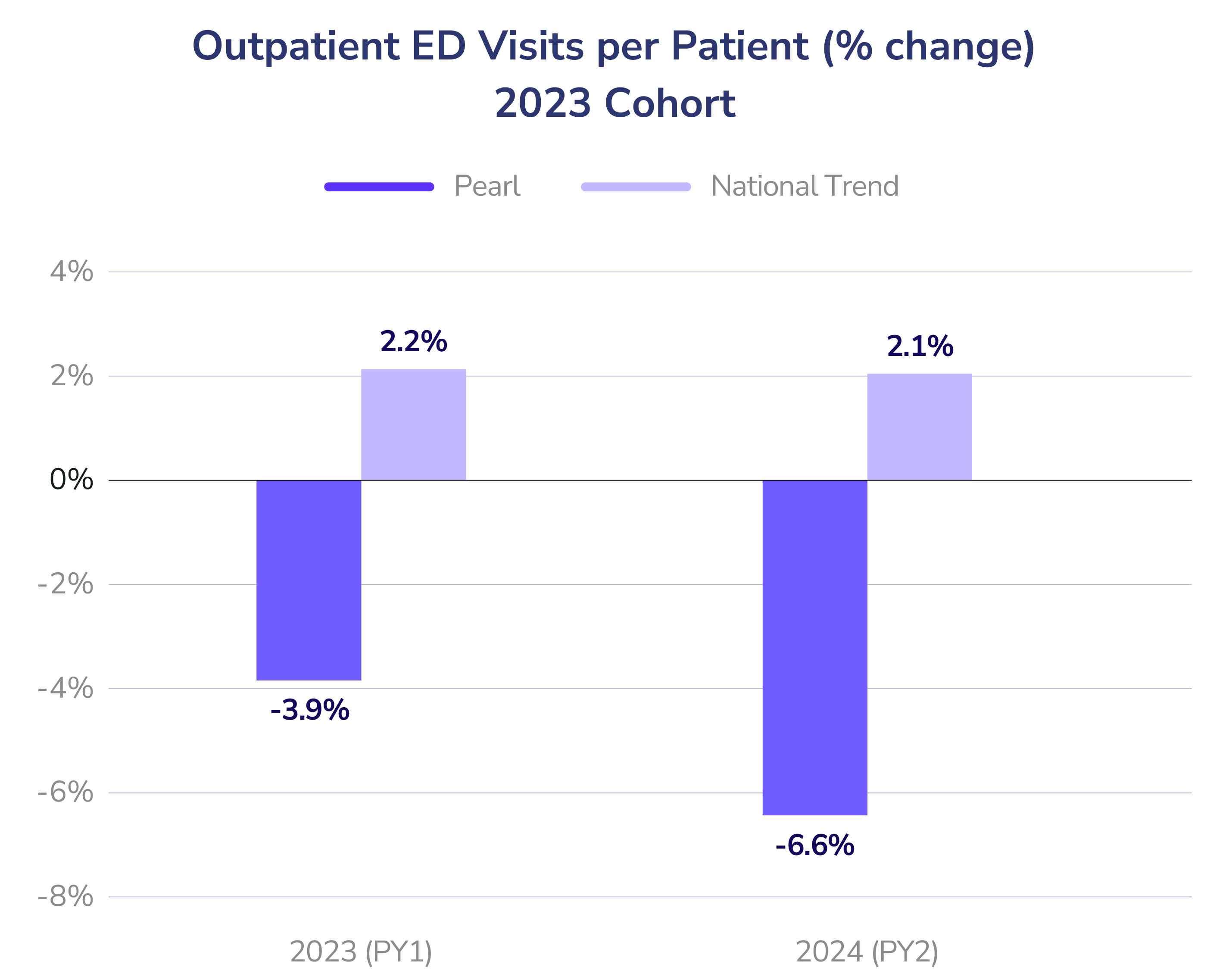
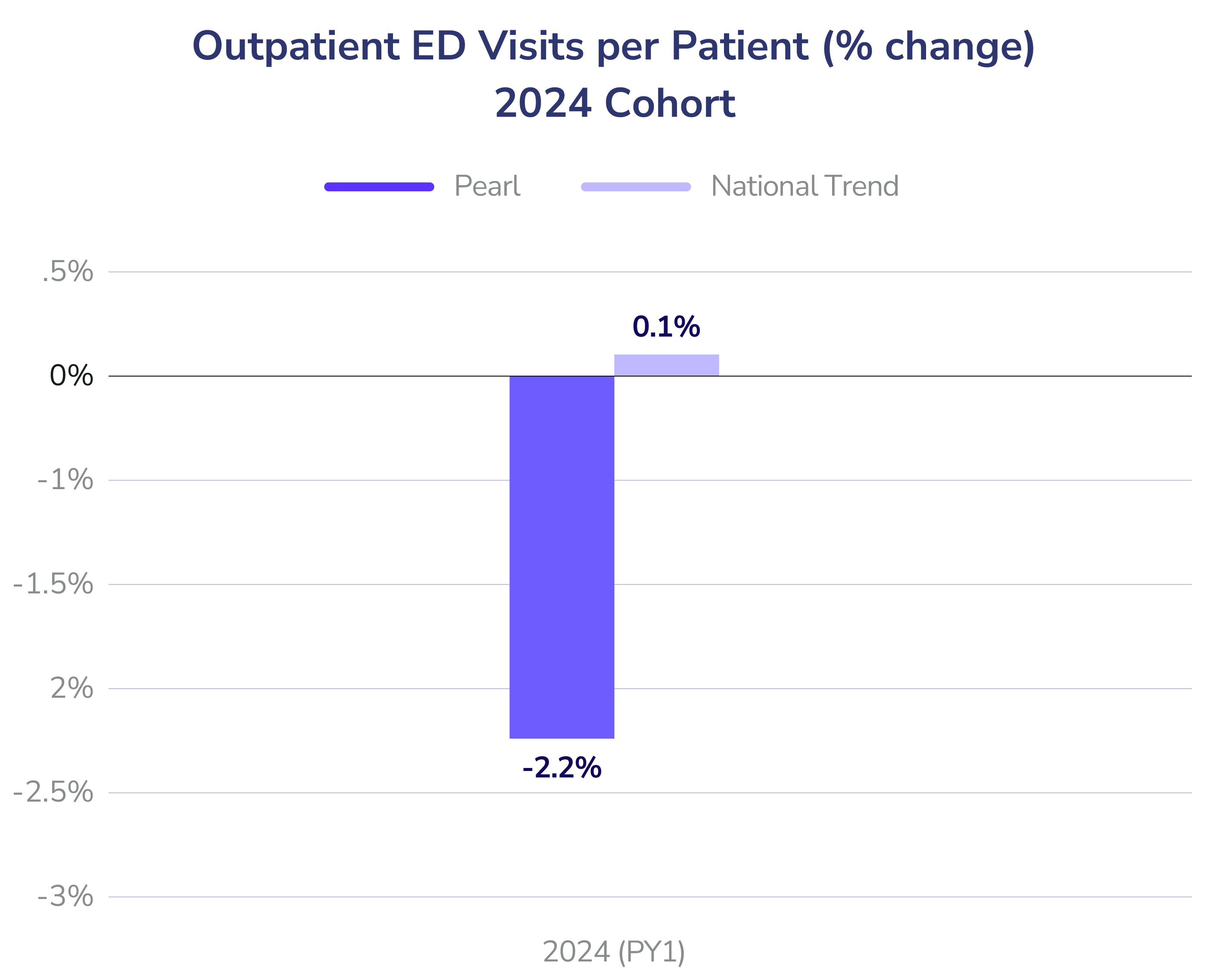
- Outpatient Emergency Department Visits per Patient: ED utilization decreased by 6% in Year 1 for the 2023 cohort and 2% for the 2024 cohort. By Year 2, the 2023 cohort was outperforming national benchmarks by 9%.
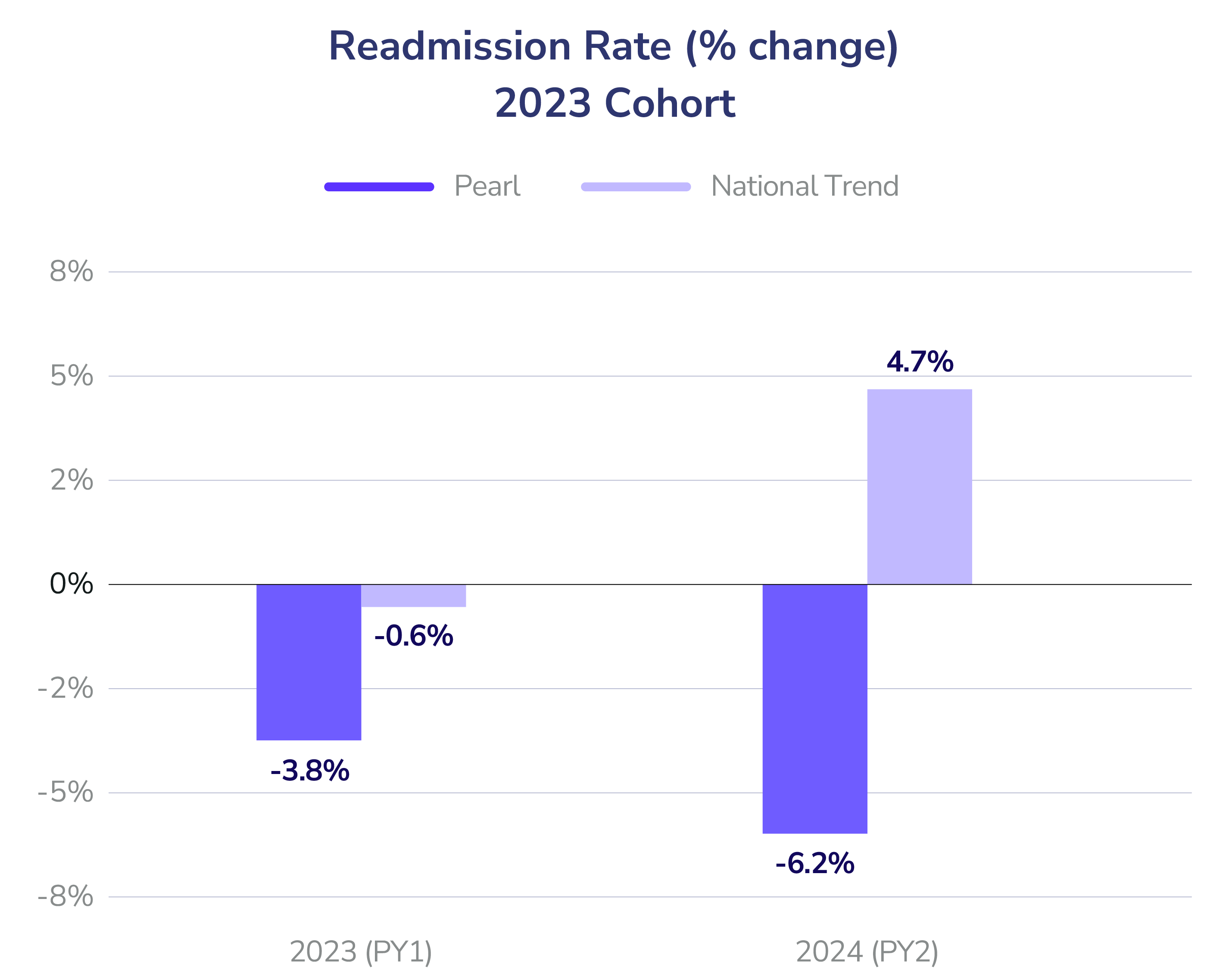
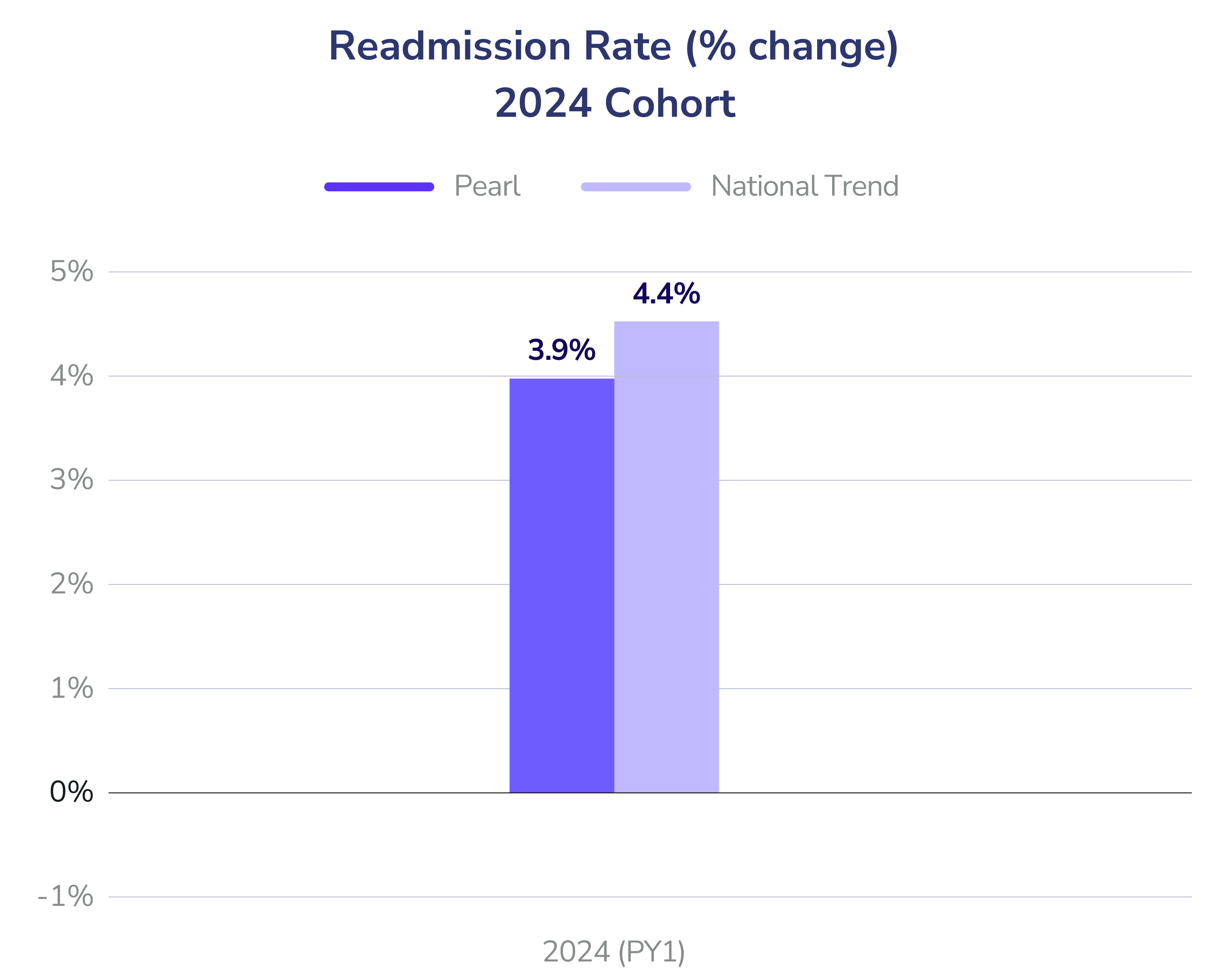
- Readmission Rates: In Year 1, reductions reached 3% (2023 cohort) and 1% (2024 cohort). By Year 2, the 2023 cohort slashed readmission rates by an impressive 12% against the national baseline.
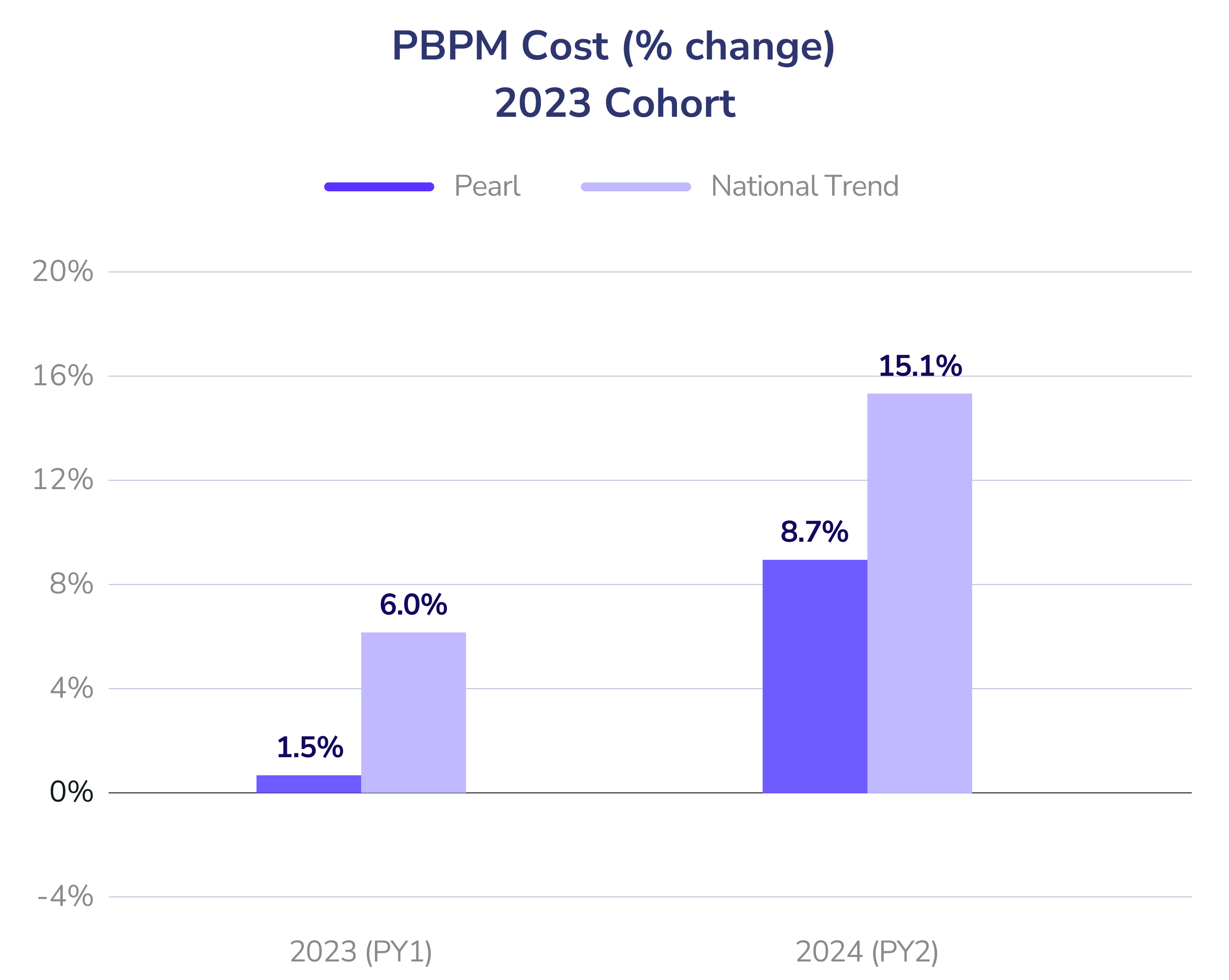
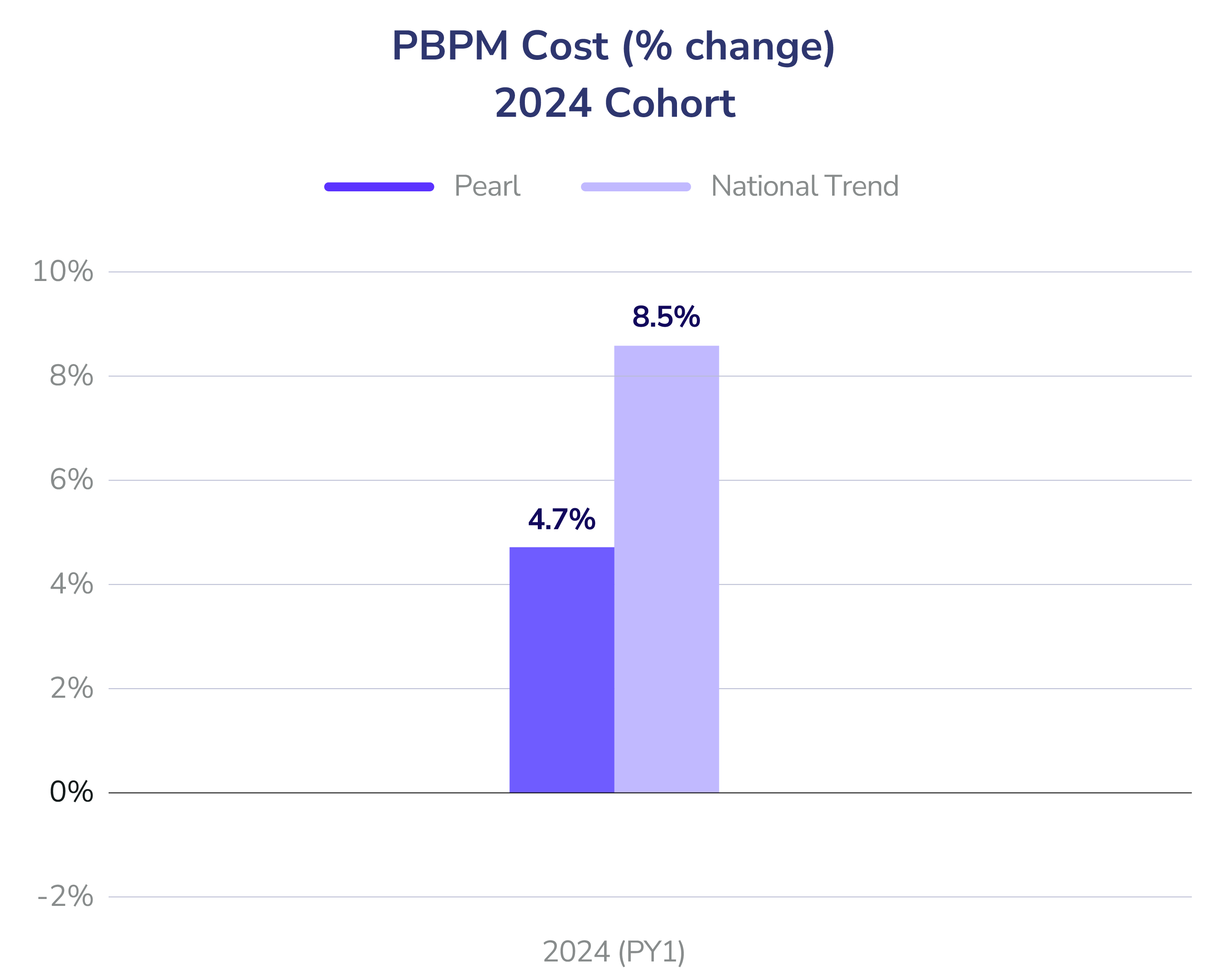
- Total Cost of Care (PBPM): Both cohorts (2023 and 2024) achieved a 4% risk-adjusted reduction in Year 1. By Year 2, the 2023 cohort widened its lead, outperforming the national benchmark by 6%.
Risk-Adjusted Utilization Trends
(% Change from Baseline)
A Partnership Built for Long-Term Success
Value-based care is not defined by short-term gains, but by whether performance holds and improves over time. What the data suggests here is not a one-time lift, but risk-adjusted improvement that continues to strengthen year over year.
By empowering primary care providers with clearer visibility, actionable insights, and care management strategies, Pearl supports ACOs and clinical organizations transform patient care while capturing the full value of their performance.
Note: The Pearl Platform empowers and enables independent clinician decision-making, never replacing it. This post does not reflect peer reviewed study results and is for informational purposes only. These results are not guaranteed. Actual results for any given practice may vary significantly.