U.S. healthcare spending reached $5.3 trillion in 20241, accounting for nearly 18% of GDP. By 2033, it is projected to exceed 20% of GDP2, further straining employers, taxpayers, clinicians, and patients alike. This is not a new story. What is new is where the next era of healthcare spending will be decided.

By 2030, 20–30% of all healthcare spend3 will be directly shaped, allocated, or guided by artificial intelligence. This will not happen because AI becomes the largest budget line item, but because it becomes the intelligence layer behind nearly every major healthcare decision.
From Tool to Control Plane
Today, AI still represents a small fraction of total healthcare spending. The direct revenue tied to AI technology in healthcare, nearly $26.6 billion in 2024, remains modest compared with U.S. healthcare’s overall expenditure, suggesting that AI products alone still account for well under 1% of total healthcare spend.
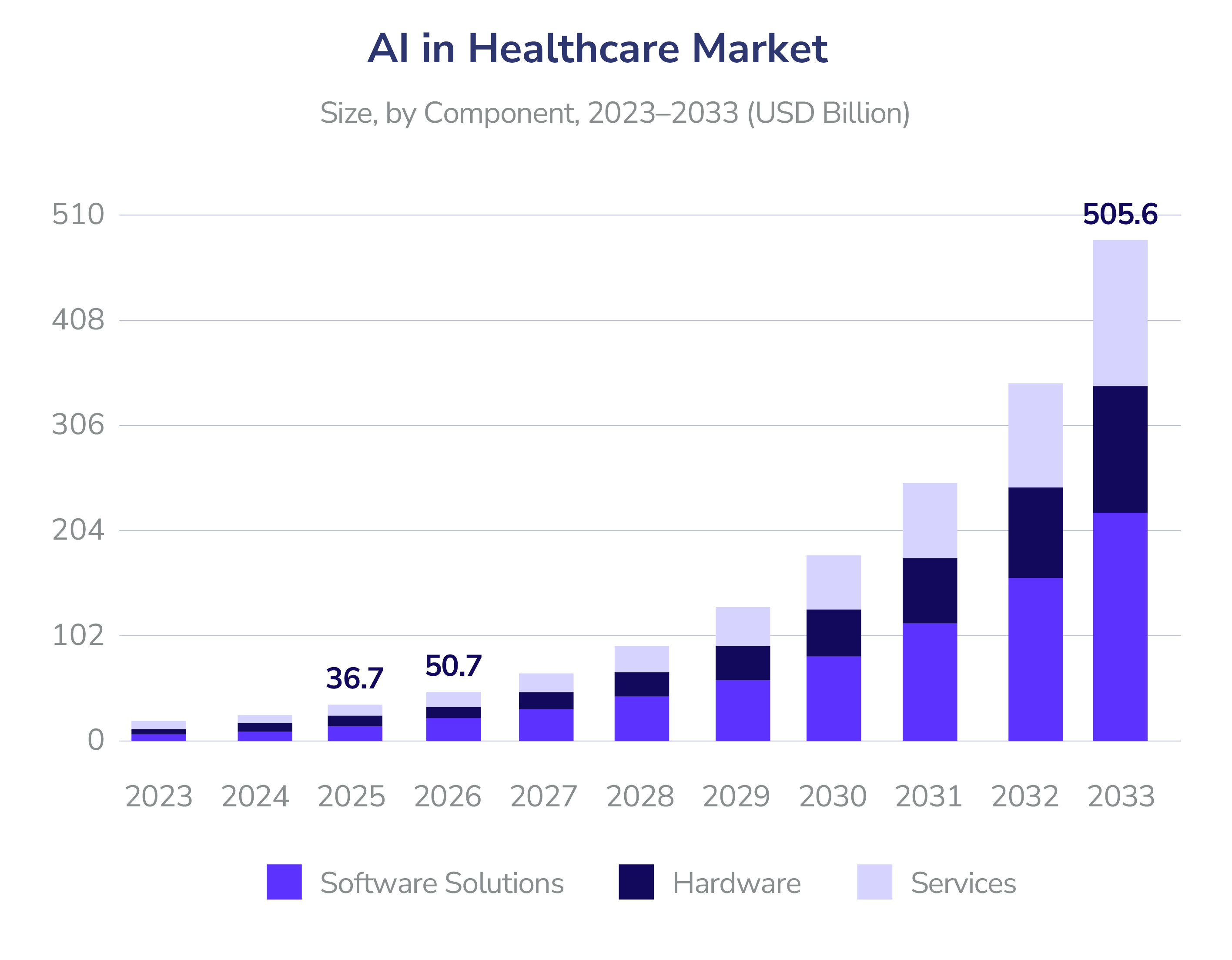
But focusing solely on AI’s direct dollar share misses the larger transformation taking place. AI is no longer just point tools or isolated automation features. According to Bessemer Venture Partners’ (BVP) State of Health AI 20264, AI is moving from early experimentation into mission-critical infrastructure for healthcare systems. This generational shift is powered by companies building AI-native products that are scaling faster, delivering stronger unit economics, and reshaping how clinical and operational work gets done.
In this new era, AI is becoming the control plane for key aspects of healthcare delivery and spending. Instead of sitting on the sidelines, AI is being integrated into administrative workflows, clinical decision support, utilization management, and even future payment mechanisms. For example:
- Administrative and revenue cycle operations: Investment and adoption in companies applying AI to automate core administrative functions are surging, with AI startups capturing an outsized share of health tech funding. In 2025, AI companies accounted for 55% of total health tech funding, up sharply from prior years. This flow of capital reflects investor belief that AI will soon dominate core administrative and workflow infrastructure.
- Clinical pathways and utilization management: Bessemer predicts a marked rise in clinical AI applications by 2026, including triage, assessment tools, and other clinician-facing AI workflows that help shape care decisions in real time, supporting more efficient utilization.
- Pharmacy optimization and adherence: While not yet quantified with a single percentage, private-market signals reveal that AI is accelerating the formation of new categories such as health AI data infrastructure and analytics platforms that can influence prescribing patterns, medication adherence, and outcomes tracking, all of which will be vital to shaping pharmacy spend.
These market trends align with broader healthcare innovation signals. Analysts and industry leaders increasingly describe AI deployments as core infrastructure, not optional features, with large health systems embedding AI across operational layers to manage cost pressures and workforce shortages.
In other words, AI is evolving from experimental pilots to a central operating layer for healthcare. The vectors of adoption and investment show that AI will increasingly be embedded in the mechanisms that decide how dollars are spent, not merely what tools are purchased. By the end of this decade, AI will meaningfully influence spending across all major domains of the system, from revenue cycle and clinical pathways to utilization management and pharmacy operations.

Who Is Actually Using AI Today?
This shift is already underway.
As of 2024, 66% of physicians reported using some form of health AI15, up from 38% the year prior. That represented a 78% year-over-year increase. Adoption is not confined to a single stakeholder group. It now spans the healthcare ecosystem.
Consumers increasingly interact with AI through virtual assistants, symptom checkers, and personalized health management tools. Virtual medical assistant revenues alone are projected to reach $2.2 billion by 20306, supporting chronic care management, appointment scheduling, and early diagnostic guidance.
Physicians are seeing the most immediate value7 in time savings and administrative relief. AI-powered ambient scribes have reduced in-visit documentation time by approximately 20% and after-hours charting by 30%8, giving clinicians back time once lost to keyboards. As a result, 57% of physicians cite administrative burden reduction as AI’s biggest opportunity.
This matters because administrative complexity remains healthcare’s largest inefficiency. Excess administrative costs add an estimated $268 billion annually9 to the system.
Care teams are deploying AI for risk reduction and proactive intervention with predictive analytics that enable more efficient and effective care coordination and resource allocation. In value-based settings, AI-enabled risk stratification can reduce hospital admissions nearly 30% by identifying high-risk patients earlier and enabling proactive intervention.
Diagnostics and procedures are also evolving rapidly. In medical imaging, AI algorithms now meet or exceed human accuracy 10, 11 in several cancer detection use cases. In surgery, robot-assisted procedures, which represent the largest AI-enabled clinical application today, have achieved success rates approaching 98% in minimally invasive contexts.
The Economic Stakes
The financial implications are substantial.
Researchers from McKinsey, building on academic analyses from Harvard-affiliated economists, estimate that widespread AI adoption could unlock up to $360 billion in annual savings across U.S. healthcare12.
- Private payers: 7–9% cost reduction, or $80–110 billion
- Physician organizations: 3–8%, or $20–60 billion
- Hospitals: 4–11%, or $60–120 billion
The sources of value are well understood. They include automating administrative workflows, reducing preventable admissions, improving utilization management, detecting fraud, and accelerating drug development. PwC projects13 that by 2035, nearly $1 trillion in annual healthcare spend will shift away from legacy cost structures and into AI-enabled operating models.
Why This Matters for Medicare
For Medicare in particular, this shift is existential.
As the population ages and clinician supply tightens, the system cannot rely on incremental labor or traditional utilization controls. The only scalable path forward is intelligence that is applied systematically, continuously, and upstream.
- Which patients receive early intervention
- Which services are delivered and which are avoided
- How care teams are deployed
- How pharmacy spend is optimized
- How outcomes are measured and improved
In practical terms, AI will decide how Medicare dollars are actually spent.
Lead or Follow
By 2030, AI will no longer appear as a standalone line item in healthcare budgets. Instead, it will be embedded in the workflows that govern spending across administration, clinical care, and pharmacy.
The real question for healthcare organizations, particularly those operating in value-based care, is not whether AI will reshape spending patterns. That outcome is already inevitable. The choice is simple: will your organization lead this existential transformation, or will you allow others to set the rules for the AI-enabled future of healthcare spending?
Connect with Pearl Health CEO & Co-founder Michael Kopko and Chief Business Officer Steven Duque on LinkedIn.
- Centers for Medicare & Medicaid Services, “NHE Fact Sheet,” last modified January 14, 2026, https://www.cms.gov/data-research/statistics-trends-and-reports/national-health-expenditure-data/nhe-fact-sheet.
- Jane Sarasohn-Kahn, “National Health Spending in the U.S. in 2033: What 20.3% of the GDP Will Be Spent On,” HealthPopuli.com, June 25, 2025, https://www.healthpopuli.com/2025/06/25/national-health-spending-in-the-u-s-in-2033-what-20-3-of-the-gdp-will-be-spent-on/.
- Grand View Research, "Artificial Intelligence In Healthcare Market Size, Share & Trends Analysis Report By Component... and Segment Forecasts, 2026 - 2033," Grand View Research, 2026, https://www.grandviewresearch.com/industry-analysis/artificial-intelligence-ai-healthcare-market.
- Bessemer Venture Partners, “State of Health AI 2026,” BVP Atlas, January 22, 2026, https://www.bvp.com/atlas/state-of-health-ai-2026.
- Tanya Albert Henry, “2 in 3 Physicians Are Using Health AI—Up 78% from 2023,” American Medical Association, February 26, 2025, https://www.ama-assn.org/practice-management/digital-health/2-3-physicians-are-using-health-ai-78-2023.
- KBV Research, “Health Intelligent Virtual Assistant Market,” KBV Research, n.d., https://www.kbvresearch.com/press-release/health-intelligent-virtual-assistant-market/.
- “Physicians’ greatest use for AI? Cutting administrative burdens,” American Medical Association.
- Maxim Topaz, Laura Maria Peltonen, and Zhihong Zhang, "Beyond Human Ears: Navigating the Uncharted Risks of AI Scribes in Clinical Practice," npj Digital Medicine 8, no. 1 (September 24, 2025): 569, https://pmc.ncbi.nlm.nih.gov/articles/PMC12460601/.
- Saraswathula A, Merck SJ, Bai G, et al. The volume and cost of quality metric reporting. JAMA. 2023;329(21):1840-1847. doi:10.1001/jama.2023.7271
- McKinney SM, Sieniek M, Godbole V, et al. International evaluation of an AI system for breast cancer screening. Nature. 2020;577(7788):89-94. doi:10.1038/s41586-019-1799-6
- Liu X, Faes L, Kale AU, et al. A comparison of deep learning performance against health-care professionals in detecting diseases from medical imaging: a systematic review and meta-analysis. Lancet Digital Health. 2019;1(6):e271-e297. doi:10.1016/S2589-7500(19)30123-2
- Davenport T, Kalakota R. The potential for artificial intelligence in healthcare. Future Healthc J. 2019;6(2):94-98. Republished by McKinsey & Company. https://pubmed.ncbi.nlm.nih.gov/31363513/
- PwC. From breaking point to breakthrough: the $1 trillion opportunity to reinvent healthcare. PwC. September 17, 2025. https://www.pwc.com/us/en/industries/health-industries/library/future-of-health.html




